Junctional escape rhythm
Inherent rates are as follows: atria–75 beats/minute AV node - 60 beats/minute ventricles–40 to 60 beats per minute and normal heart rate - 60 to 100 beats per minute. The rhythm would then be called a junctional escape rhythm. If higher pacemaker sites fail, a junctional escape pacemaker might take control of the heart. NOTE: The normal inherent rate of atrial ventricular junction is 40 to 60 beats per minute. What happens is that the AV node takes over the pacemaking function. (4) The QRS complex lasts less than 0.12 of a second. (3) The PR interval can only be measured if the P wave precedes the QRS Complex. (2) P waves will be inverted and can fall before, during, or after the QRS complex. The regularity depends on the regularity of the underlying rhythm and the rate depends on the rate of the underlying rhythm. Junctional escape rhythm: 40-60 BPM Accelerated junctional rhythm: 60-100 BPM Junctional tachycardia. A wave of depolarization spreads out from the ectopic focus and causes a premature contraction. Occurs when the rate of an AV junctional pacemaker exceeds that of the sinus node Arises when there is increased automaticity in the AV node coupled with decreased automaticity in the sinus node Junctional rhythm classification by rate. The abnormal impulse is generated from the region of the heart called the ectopic focus. This causes an occasional abnormal impulse to be generated between the normal impulses. (1) Premature junctional contraction is another form of heart abnormality. This condition occurs when a small region of the heart becomes more excitable than normal. Analysis of premature junctional contraction (PJC) is given below and an example is shown in figure 1-21. Accelerated junctional rhythm: 60 to 100 BPM. Types of junctional rhythm include: Junctional bradycardia: Less than 40 BPM. All junctional rhythms will create an inverted P wave, but some low atrial impulses can also cause inverted P waves.ī. Junctional rhythm can cause your heartbeat to be slower than normal (bradycardia), or faster than normal (tachycardia). An inverted P wave can occur before, during, or after the QRS complex. These abnormal conditions will depolarize the ventricles in the normal manner (normal QRS). Junctional arrhythmias create an inverted P wave because the atria are depolarized by the retrograde conduction. Cardiac and non-cardiac causes of T-wave inversion in the precordial leads in adult subjects: A Dutch case series and review of the literature. Said SA, Bloo R, de Nooijer R, Slootweg A.Left anterior hemiblock or inadvertent lead misplacement? Chest. Sinoventricular Conduction in the Setting of Severe Hyperkalemia. Tall R in aVL may appear like left ventricular hypertrophy. This ECG also looks like right ventricular hypertrophy at one look of V1 and V2.
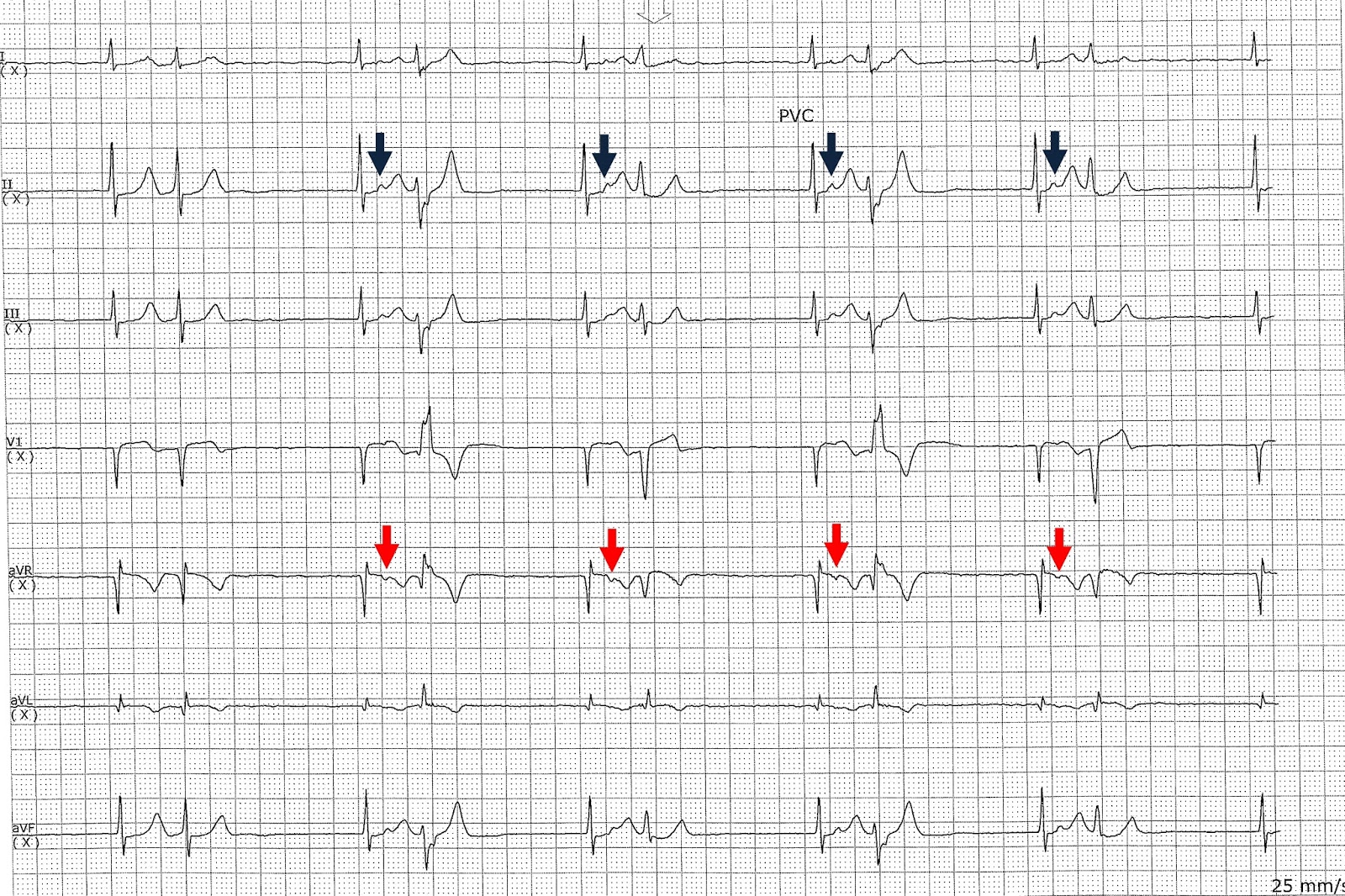
Hemiblocks may simulate or conceal the ECG findings of myocardial infarction or ischemia and mask or simulate ventricular hypertrophy. The concept of trifascicular intraventricular conduction was introduced by Rosenbaum MB et al in 1968. Beats 5 and 8 have P-like deflections immediately preceding the QRS. There appear to be P waves preceding some, but not all, beats (all except 5 and 8). The ECG shows an irregularly irregular rhythm that is slightly bradycardic but nearly normal in rate (Figure 1). Arrow head T inversion in aVL seems to be a primary repolarization abnormality ( primary T wave abnormality), indicating myocardial disease like ischemia or injury. Answer: Normal sinus rhythm with junctional escape beats. T wave inversion in V1 and V2 can be secondary repolarization abnormality due to change in depolarization sequence due to right bundle branch block (secondary T wave abnormality). Minor difference between two QRS complexes in V2 and V3 are also seen. The difference in pattern between two QRS complexes in V1 is difficult to explain. qR pattern in I and aVL also go with left anterior hemiblock. RBBB and LAHB together constitute a bifascicular block. Delay in septal activation can produce q waves in V1 and V2 in LAHB even without anterior wall myocardial infarction.

Other findings in the ECG are left axis deviation with rS pattern in inferior leads suggesting left anterior hemiblock (LAHB) and qR pattern in V1 and a slurred S in V6 indicating right bundle branch block (RBBB). If the baseline artefacts are ignored, it becomes a pure junctional rhythm.Īlternate possibility in view of the tall peaked T waves (pink arrows) is an atrial paralysis with sinoventricular conduction in hyperkalemia. If the baseline artefacts are considered as fibrillary waves, then it has to be considered as atrial fibrillation with complete heart block and a junctional escape rhythm. Though there are some baseline artefacts, no definite P waves or fibrillary waves are seen. RBBB with LAHB & Junctional rhythm: ECG shows a slow regular rhythm with a ventricular rate of around 43/min.
